Miscellaneous
Fanning out first responders far and wide
In a major earthquake when the collapsed buildings also include the only health institute in an affected area, problems brought about by the disaster get accentuated.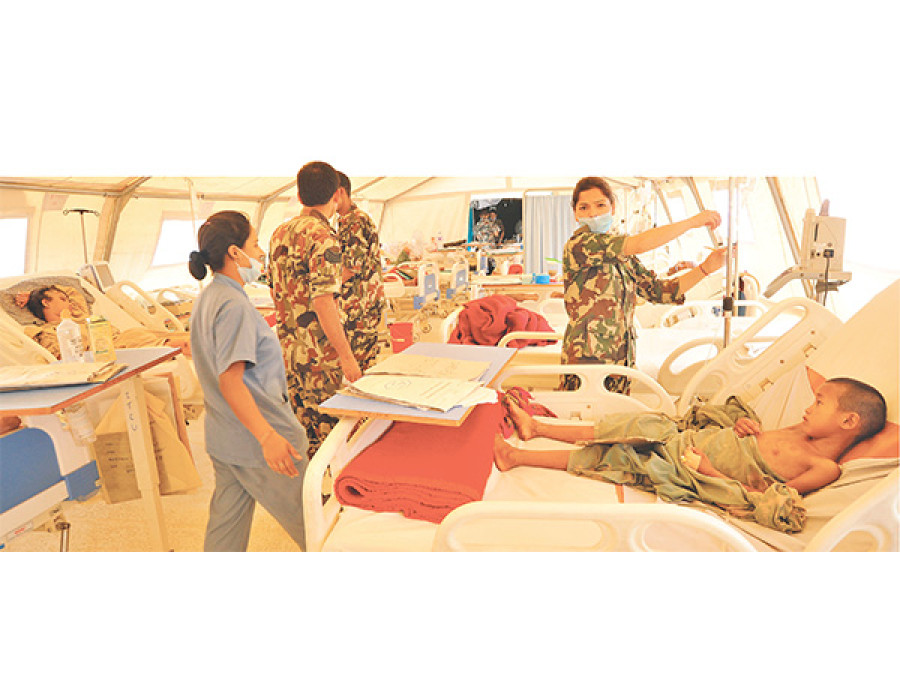
Manish Gautam
The Great Earthquake on April 25 revealed the vulnerable state of our health institutes, especially of those in rural areas. Most of the health centres in the 14 worst-affected districts collapsed, showing that the countryís plans on disaster preparedness were focused maybe a tad too heavily on urban areas.
The tag ëthe worst-affected districtí means that the people in the thus-labled districts are the ones who need (immediate) medical attention the most. In the first few days, if not hours, after an earthquake, access to a sound healthcare system becomes a matter of life or death in these areas. A slight delay in treating patients could lead to permanent disability or death. Even seemingly minor wounds, if infected and left untreated for too long, can result in severe cases of disability.
A small source of comfort in the wake of the Great Quake was that some of the government, private and community hospitals inside and outside the immediate vicinity of the Kathmandu Valley performed exceptionally well. But as the frequency of the aftershocks winds down and life limps back to normalcy, the government must review its medical-response strategy and prepare its workforce for serious calamities that might occur in the future—not just in the centre, but across the nation as well. One way to go would be to establish more` medical colleges nationwide; the other would be to better utilise the ones we already have in districts by turning them into disaster-response centres.
Ideas about the equitable distribution of healthcare had already been gaining ground for some time even before the earthquake struck on April 25. For quite some time now, medical professionals have been asking the government to establish medical colleges throughout the country on the basis of geography and the size of populations. Dr Govinda KC, a senior orthopaedic surgeon, brought this demand to the limelight when he staged a fast-unto-death protest five different times in the recent past.
The establishing of a medical college in a new area, say experts who profess a similar school of thought, increases the number of doctors, medical interns and other medics required to respond immediately in times of disaster in that area. Since a medical college must have operation theatres and around 800 beds, doctors can also handle cases more efficiently in such facilities in the wake of disasters.
ìMedical colleges cannot be established overnight. But if we donít begin working on opening them right now, it will delay the process further,î says Dr KC.
Dr KC is one of the very few doctors in the country who has tended to disaster victims across the world. He has vast experience working with patients in underdeveloped nations, where healthcare systems easily get overwhelmed at times of big calamities. What Dr KC finds is a pattern that is common in all developing nations: in the lack of immediate medical attention, the poor patients end up becoming permanently disabled, adversely affecting their chances of making socio-economic progress afterwards and creating a vicious loop in which the victims find themselves trapped in poverty.
But if establishing new medical colleges can wait, at least according to some who donít want to go the route, making the existing medical schools socially accountable cannot. Making them so would entail bringing all the existing medical colleges in line with the government system and compelling them to choose at least one district to deliver health services.
ìIn this system, the medical college will make an arrangement to provide at least one specialist, one medical officer, a mandated number of nurses and other paramedics to a healthcare centre in a chosen district,î says Dr Jagdish Prasad Agrawal, a medical educator. ìThis team will work at the health centre for at least a month before being replaced by another similar team from the same medical college. And this goes on until we find a better alternative.
So far, only some of the institutions have implemented this model of medical practice. The IOM has a health centre in Chautara, Sindhupalchok—the district worst-hit by the April 25 earthquake—where doctors make their rounds accompanied by post-graduate students.
If other medical colleges could be brought under this system immediately, people in the affected area would get prompt medical attention in times of future disasters. The burden on big hospitals in urban areas would be reduced, and young students would also get a chance to interact with communities and learn better about the challenges doctors face in the districts. ìBesides, for the patients, getting treatment in nearby hospitals or health centres, with family members around, has its own psychological benefits,î says Dr Agrawal.
But even if a medical college were to be established in each district or even if their team were to work in cycles in a centre in a district, a disaster like the Great Quake could easily overwhelm the healthcare system. An international support team could, no doubt, help reduce the volume of patients a doctor sees in times of crisis, but it takes at least 48 to 72 hours for such a team to even arrive at the scene of impact.
If we canít build hospitals around the country at the needed clip, we can at least have an emergency national medical team on standby. This team should have the authority to access the devastated sites immediately and make its way to the place that needs the support the most. This team could have many other teams under it, but each team has to be deployed immediately where it is needed most, and not just focus on the centre. But whatever solution the nation comes up with to enable better response to earthquakes, the solution must be thought up soon. As our health system recovers from the jolt it received from the Great Quake, policymakers must make arrangements, post haste, say experts like Dr KC, to deal with future calamities more effectively.




 22.12°C Kathmandu
22.12°C Kathmandu










