Health
Fresh black fungus cases down but might emerge if Covid-19 flares, doctors warn
The main drug for the treatment of black fungus is not available after India’s export ban and treatment is very expensive.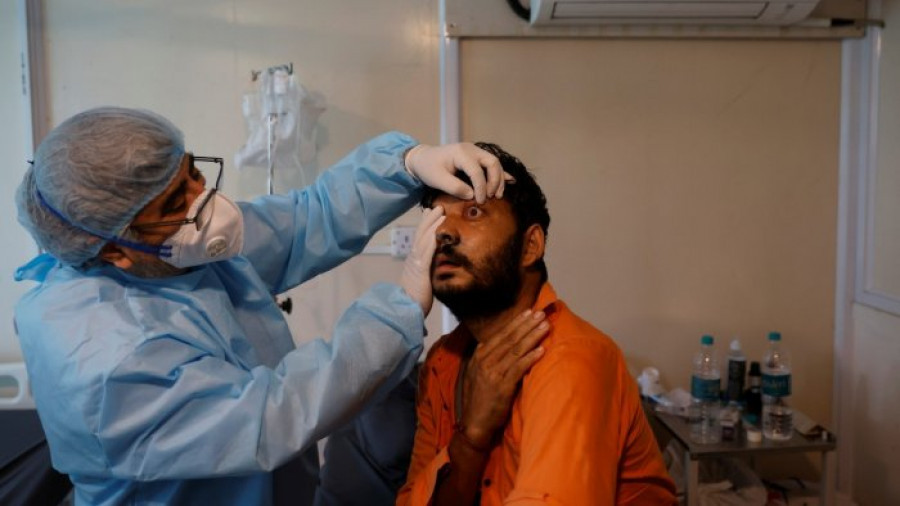
Prithvi Man Shrestha
The Tribhuvan University Teaching Hospital currently has been treating just three patients of mucormycosis, a rare fungal infection commonly known as ‘black fungus’ and mostly found among diabetic Covid-19 patients.
Along with the reduction in Covid-19 cases, the hospital has not received new patients of mucormycosis for nearly a month. But, the hospital has so far treated 18 patients of black fungus and a majority of them were admitted to the hospital in May and June.
“Two patients died, we sent five patients home making them clear that they cannot be fully cured, three are getting treatment at the hospital and the rest have recovered from the disease,” Dr Rabindra Pradhananga, coordinator of the Mucormycosis Management Committee at the Teaching Hospital.
Likewise, there is no mucormycosis patient admitted at the Unified Covid-19 Hospital, run on the premises of Bir Hospital.
“We had six patients with mucormycosis. Of them, three died and three recovered,” Dr Nabin Pokharel, deputy director at the Unified Covid-19 Hospital told the Post.
Mucormycosis affects the brain, sinuses and lungs and can be life-threatening to diabetic or severely immunocompromised individuals like cancer and HIV/AIDS patients. Such cases have appeared mostly among Covid-19 patients in Nepal and neighbouring India.
According to the Ministry of Health and Population, around two dozen cases of mucormycosis have been found across the country so far. “Of them, 18 received treatment with the government’s support,” said Krishna Prasad Paudel, spokesperson at the ministry.
The black fungus infection is mostly seen in people with pre-existing diabetic conditions who have been infected with the coronavirus. It causes blackening or discoloration over the nose, blurred or double vision, chest pain, breathing difficulties and coughing blood.
The indiscriminate use of steroids for some Covid-19 patients could be linked to mucormycosis or other fungal infections, doctors say.
While the number of new black fungus cases is not being found lately along with the reduction in Covid-19 cases since June, doctors said that new mucormycosis cases might emerge again if the Covid-19 cases again rise substantially. There are already indications that the Covid-19 cases are fast rising and the most deadly variant of Covid-19 called ‘Delta’ is circulating in the population.
According to a statement issued by the Health Ministry on Tuesday, of the 47 swab samples of the infected persons collected between early June and mid-July, on which whole-genome sequencing were performed in the World Health Organisation-identified Center for Excellence in Genomics, the Institute of Genomics and Integrative Biology in Delhi, Delta variant (B.1.617.2) was found in all swab samples and new sub-lineage of it—K417N also known as AY.1, also known as Delta Plus—was found in three of them.
On July 4, the Ministry of Health and Population reported 1,042 new coronavirus infections. But, lately, the number of cases is rebounding along with gradual relaxation in lockdown that began in mid-June.
On Wednesday, Nepal reported 2,634 Covid-19 cases confirmed through polymerase chain reaction (PCR) tests and 1,206 cases were confirmed through antigen tests, according to the Health Ministry. On Tuesday, 2,726 new cases were confirmed through PCR tests while 1,173 cases were identified through antigen tests. Even during the first wave of the pandemic, the number of Covid-19 cases had surged after the lockdown was lifted from July 22 last year.
“We have to be watchful about the potential rise in mucormycosis patients if Covid-19 cases go up continuously or the country is hit by the third wave of the pandemic,” said Dr Pokharel. The potential increase in black fungus cases is concerning even from the point of view that there is hardly any vial of the Liposomal Amphotericin B, the main drug to be used in the treatment of mucormycosis patients, is available in the market.
“On the one hand, the drug is not available in the Nepali market. On the other hand, it is very expensive and most people cannot afford the drug,” said Dr Pradhananga. “Even a single vial of Liposomal Amphotericin B could cost up to Rs60,000 in the international market.”
According to a report in CNN this week, a single vial of this drug is being sold for around $95 in India. But, the southern neighbor has banned its export since early June. In a notification dated June 1, the Directorate General of Foreign Trade under India's Commerce Ministry categorised Amphotericin B under the restricted category for export with immediate effect.
According to Pradhananga, an adult may require 7-8 vials of this medicine in a day and one has to pay from Rs250,000 to Rs300,000 in a day for the drug only.
Primarily due to the shortage of this drug, Nepali doctors have been providing alternative drugs such as Deoxycholate and Posaconazole which are available in the Nepali market to treat patients with mucormycosis.
“A tablet of Dioxicoltin B costs Rs1,600 and a tablet of Posaconazole costs Rs1000 and its three doses are needed for a black fungus patient daily,” said Dr Pradhananga. If the injection is used, a vial of Posaconazole costs around Rs16,000.”
According to him, Dioxicoltin B used for his black fungus patient has side effects such as creating problems in the kidney and arouses hypersensitive reactions. So, he suggested that the best option for patients would be to make available Liposomal Amphotericin B at a cheaper price.
According to Dr Pokharel, the Unified Covid-19 Hospital has just a few vials of Liposomal Amphotericin B remaining which may be enough to treat one or two patients only.
Even though the government had received 1,000 doses of Liposomal Amphotericin B in early June from the World Health Organization (WHO), almost all of them were used up by the end of that month. The government had distributed the drugs to different government-owned hospitals for the treatment of this disease.
According to the Ministry's spokesperson Paudel, the ministry is trying to get additional doses from the WHO. “Our stock for free distribution is out and we are trying to get additional doses from the WHO,” he said.
Black fungus cases had started to appear in Nepal in May. A patient who was hospitalized at Lumbini Provincial Hospital died in late May. Another patient who had been admitted to Seti Zonal Hospital died on June 3. In May, four Covid-19 patients were found with the black fungus infection at the Nepalgunj-based Bheri Hospital of which one had died.




 24.12°C Kathmandu
24.12°C Kathmandu















