National
As black fungus cases rise, country faces shortage of drugs for treatment
India has put a ban on export of the drugs. So far around two dozen cases of black fungus among diabetic Covid-19 patients and at least six deaths have been reported.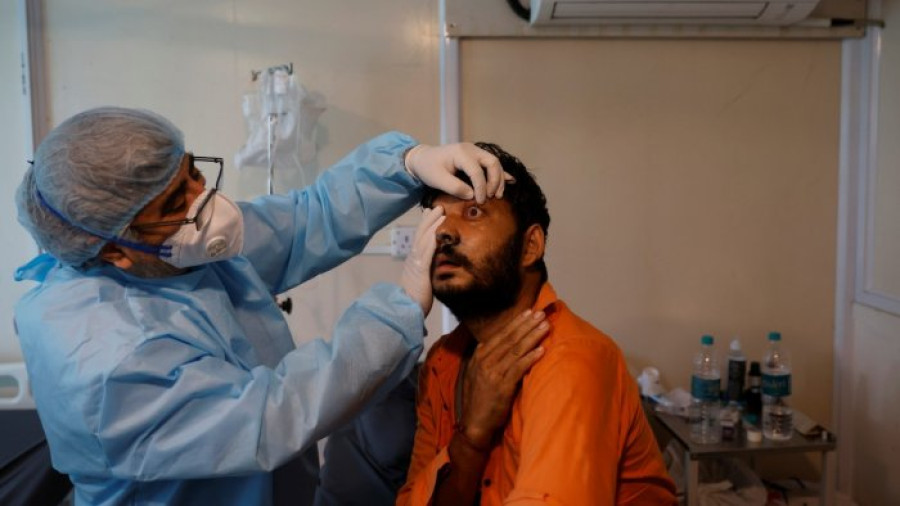
Prithvi Man Shrestha
The Tribhuvan University Teaching Hospital on Saturday admitted two new patients—a 56-year-old woman and a 65-year-old man—with mucormycosis, a rare fungal infection commonly known as ‘black fungus’ and mostly found among diabetic Covid-19 patients.
With the new cases, the number of patients with mucormycosis at the government-run hospital has reached 14.
According to the hospital, the condition of both patients admitted on Saturday is critical.
But the hospital does not have Liposomal Amphotericin B, the primary drug used for treating the black fungus infection.
India, the main source of the drug, has banned its export.
“In the absence of this drug, we are treating the patients with an alternative drug—Deoxycholate,” said Dr Rabindra Pradhananga, coordinator of the Mucormycosis Management Committee at the Teaching Hospital.
Mucormycosis affects the brain, sinuses and lungs and can be life-threatening to diabetic or severely immunocompromised individuals like cancer and HIV/AIDS patients. Such cases have appeared mostly among Covid-19 patients in Nepal and neighbouring India.
Amid the shortage of Liposomal Amphotericin B, Deoxycholate and Posaconazole are two other drugs available in the Nepali market to treat patients of mucormycosis.
But Dr Pradhananga said that the patients’ families need to procure Deoxycholate and Posaconazole from the markets and these drugs are available only because they were in stock before India imposed a blanket ban on the export of Amphotericin B drugs amid surging cases of mucormycosis in India in early June.
“All three drugs—Liposomal Amphotericin B, Deoxycholate and Posaconazole— come under Amphotericin B and all of them come under India’s restrictive category,” said Dr Pradhananga.
The government does not have any of these drugs in its store to distribute to its hospitals at the moment.
“We had received 1,000 doses of Liposomal Amphotericin B in early June from the World Health Organization but they have been used up,” said Krishna Prasad Paudel, spokesperson at the Ministry of Health and Population. “Alternative drugs can be found in the market but they are not as good as Liposomal Amphotericin B. The government does not have a stock of these alternative drugs either.”
In a notification dated June 1, the Directorate General of Foreign Trade under India's Commerce Ministry categorised Amphotericin B under the restricted category for export with immediate effect.
According to an NDTV report as of June 11, over 31,000 black fungus cases had been identified in India with the death of over 2,100 people from the infection.
With the stock of the Deoxycholate and Posaconazole also running out in the market, doctors said that it would be difficult for Nepali patients to secure these drugs if cases of black fungus rose sharply.
A patient needs many vials of this scarce drug and the 1,000 vials of Liposomal Amphotericin B received from the World Health Organization in early June were used up early.
“All the vials of the medicines were spent in treating 16 black fungus patients at government-run hospitals,” said Paudel, who is also the director of the Epidemiology and Disease Control Division under the Health Ministry. “A single patient required as many as 80 vials.”
According to him, the government had requested 3,000 vials with the WHO but only received 1,000.
Unified Covid-19 Hospital, run on the premises of Bir Hospital, also treated four patients of mucormycosis and most of the drugs made available by the Health Ministry were used, the hospital authority said.
Dr Nabin Pokharel, deputy director at the Unified Covid-19 Hospital, said that his hospital has a few vials of Liposomal Amphotericin B remaining to treat any new patients.
“Initially, we failed to get Liposomal Amphotericin B to treat patients and used alternative drugs,” said Pokharel.
The drugs to treat mucormycosis are expensive, which the poor will not be able to afford.
According to an Indian media report, one vial of Amphotericin B costs as high as INR (5,000-6,000) or almost Rs10,000 in the Indian market.
“If a patient needs 80 vials, he or she will end up paying around Rs800,000 for this medicine only,” said Paudel.
Given the shortage of the medicine in the market, the cost might be even higher in the black market.
Meanwhile, the number of black fungus cases has been rising. In early June, the fungal infection was seen in about a dozen people. Now, the number has reached around two dozens even though the number of daily new coronavirus infections in the country has been falling sharply.
On Sunday, 1,353 new Covid-19 cases were reported, the second lowest figure since April 20. On Saturday, 1,174 new cases were reported. The Ministry of Health and Population reported 34 more deaths from Covid-19 complications, taking the total toll to 9,009. The number of cases reported since the pandemic began stands at 633,679. The number of active cases stands at 40,336.
The black fungus infection is mostly seen in people with pre-existing diabetic conditions who have been infected with the coronavirus. It causes blackening or discoloration over the nose, blurred or double vision, chest pain, breathing difficulties and coughing blood.
The indiscriminate use of steroids for some Covid-19 patients could be linked to mucormycosis or other fungal infections, doctors say.
“Of the 14 patients admitted at the Teaching Hospital, one died and six were discharged, four of them after recovery and two without completing treatment as per their own request,” said Dr Pradhananga.
The other seven are undergoing treatment.
The Tribhuvan University Teaching Hospital has so far conducted surgeries on seven mucormycosis patients to remove the mucor fungus.
Likewise, two patients admitted at Unified Covid-19 Hospital have died while two others were discharged, according to Dr Pokharel.
One patient who had been admitted at Seti Zonal Hospital died on June 3. A patient who was hospitalised at Lumbini Provincial hospital died in late May.
In May, four Covid-19 patients were found with the black fungus infection at the Nepalgunj-based Bheri Hospital of which one had died.
But with the Indian ban on exports, it is uncertain when the drugs treating the disease will be available in Nepal.
“It is not certain when we can get additional vials,” said Paudel, the spokesperson.




 24.12°C Kathmandu
24.12°C Kathmandu















