Opinion
Let us spray
As there is no vaccine or treatment for Zika virus, prevention is the only option we have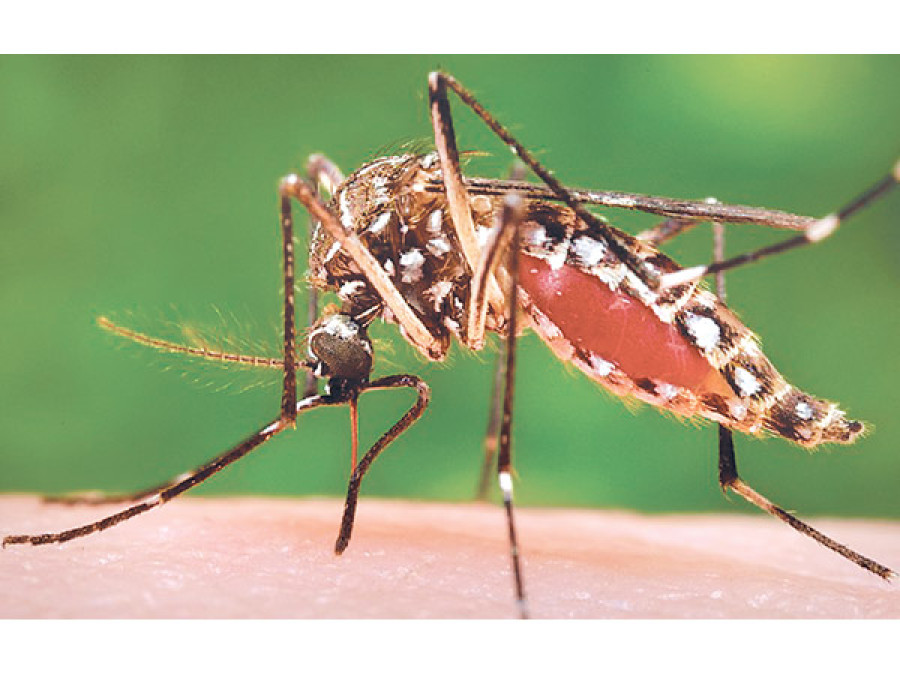
Sameer M Dixit
The Zika virus disease is spread by the Aedis mosquito species, including Aedis aegypti, Aedis albopictus and others. First identified in monkeys in Uganda in 1946, this zoonotic virus has over time been observed in countries with tropical climate in Asia, Africa and the Americas. The virus is now a topic of public health concern with the World Health Organisation (WHO) declaring it a Global Public Health Emergency of International Concern. It is indeed spreading very fast, and has affected most of the countries in Latin America, especially Brazil where more than 1.5 million people have been infected. There have been reported cases in the US too.
The disease itself is not fatal in a majority of the cases, with symptoms lasting less than a few weeks. But the biggest threat the Zika virus poses is to pregnant women with a possible link to microcephaly in newborn children born to mothers infected by the virus. Microcephaly is a condition where babies are born with a smaller than normal head which leads to other health complications as the child grows older. In Brazil alone, cases of microcelphy among newborns are around
4,000 and increasing. However, a scientifically validated link between microcephaly and the Zika virus infection is not yet available. Recently, in a study involving more than 100,000 children over four years in Brazil, microcephaly has been observed in many infants in the absence of the Zika virus. Similarly, in the US alone, which has not yet had an outbreak of Zika, there are 25,000 cases of microcephaly reported every year.
Unprotected sex
The Zika virus is a Vector Borne Disease (VBD), meaning that it requires a vector (mosquito) to take it to its host (in this case humans). Symptoms of Zika are similar to those of other mosquito-borne diseases’ such as dengue and chikungunya, which are also spread by the Aedis mosquito. Thus prevention of Zika follows the same pattern as for other mosquito-borne diseases, such as using nets and repellents, and spraying water sources with insecticides, among others. However, a major departure for Zika infection from other similar VBD infections is that the Zika virus appears to be transmittable between humans by bodily exchanges of fluids, including semen. Thus, unprotected sex poses a risk for transmission.
Whether we should worry about Zika in Nepal is a question that is being discussed by the public health sector and community in the country. At this very moment, the risk of Aedis mosquito harbouring the Zika virus is not likely present in Nepal due to the cold weather. But Zika has been identified in India in the past and chances are that the Tarai region probably has had undetected cases already. Proximity to India and exposure to Zika in the Indian population does put Nepal at increased risk of outbreaks. As long as India does not report it, we are most likely safe from transmission. However, if a Zika virus outbreak is reported in low-lying northern and eastern Indian states (Bihar, Uttar Pradesh and West Bengal), Nepal needs to be alert. Officials from our epidemiology department should therefore be coordinating with their Indian counterparts on a daily basis to keep track of what is happening across the border.
Safety measures
In light of all this, it should be pointed out that dengue and chikungunya, caused by similar viruses transmitted by the Aedis mosquito, regularly affect the population in the Tarai region bordering northern and eastern Indian states. As such, vector control is something Nepal has plenty of experience with. Mosquito-control programmes as part of prevention against malaria and dengue already exist in Nepal. Thus, the Ministry of Health in collaboration with the WHO should ensure that such programmes receive further attention as the weather gets warmer, especially in the Tarai region. Further, with even hilly cities such as Kathmandu having warmer weather during summers than earlier, they cannot be considered risk-free anymore. We have already had cases of Aedis-caused dengue in Kathmandu in the recent past. Highly populated towns and cities, including those in the hilly region, therefore also need to ensure that preventive measures are in place.
Most importantly, in light of scientific reports suggesting health risks to newborn children, health authorities in the country should focus on ensuring that pregnant women are provided safety measures such as nets, and a mosquito-free environment. Condom promotion might have to be reinforced in the Tarai region where risks of infection and transmission are high. Mechanisms to control sexually transmitted diseases already in place should be strengthened for prevention of sexual transmission of the diseases.
Since there is neither a vaccine for the virus, nor treatment regimens to control the virus in humans, prevention is the only option we have at the moment. If we use existing mechanisms of prevention already present in the country, it should be adequate to control the spread of the disease, should it ever make its way into Nepal.
Dixit is Director of Research at Center for Molecular Dynamics Nepal, Kathmandu




 25.12°C Kathmandu
25.12°C Kathmandu










