Health
Hard-to-reach populations exist not only in remote areas but also cities
Health workers say even elected officials do not comply with rules and thousands of city residents don’t trust health messages.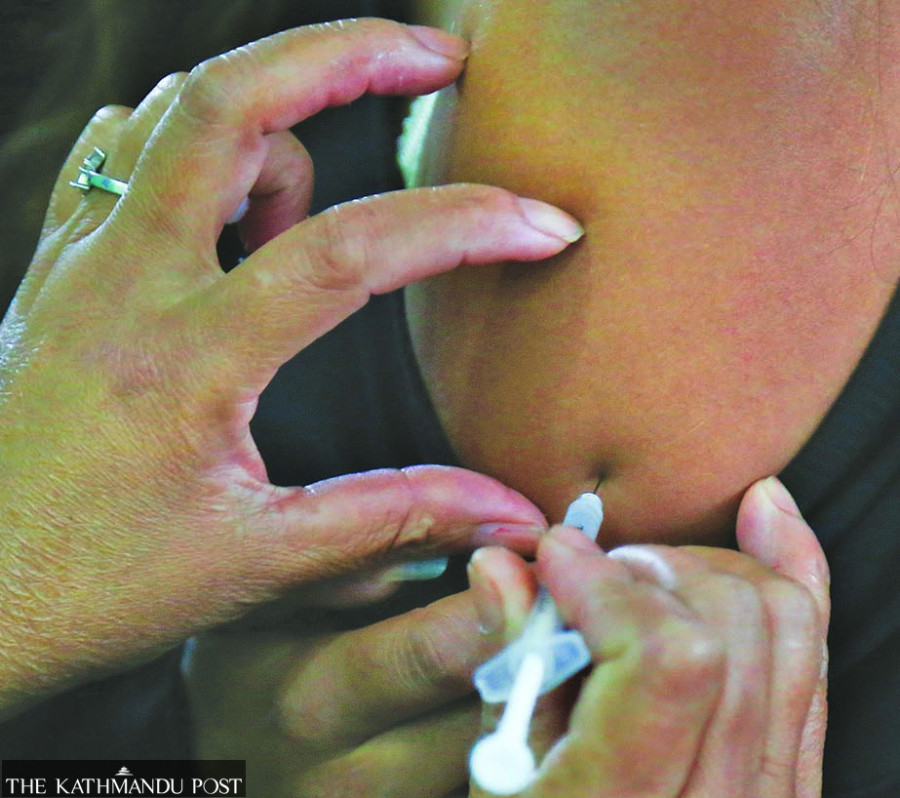
Arjun Poudel
For the last 12 years, the Ministry of Health and Population has been launching a mass drug administration programme against lymphatic filariasis or elephantiasis in Banke district.
But the Ward 16 chairman of Nepalgunj Sub-metropolitan City took the medicine for the first time this year.
“This time also he did not take the medicine on his own. Chairman of the district coordination committee insisted at a meeting that he receive the medicine,” Durga Gautam, focal person of the mass drug administration programme in the Health Office Banke, told the Post, over the phone from Nepalgunj. “Other two ward members in the sub-metropos refused to take the medicine. We could not convince them.”
Banke is one among 10 districts where the prevalence of lymphatic filariasis or elephantiasis is very high. Despite the continuation of the campaign for 12 years in a row, the prevalence of the disease has not lessened notably.
And what is concerning is that the hard-to-reach population is not only in the remote villages of far-flung districts but a significant number of them are in big cities and towns.
According to Gautam, the ward chair who took the medicine for first time and the ward members who refused to take the medicines are from the Muslim community.
“They refused not only to take the medicine but also to ask others in their family and neighbourhood to take the medicine,” said Dr Gokarna Dahal, an official at the Epidemiology and Disease Control Division. “Even the Muslim religious leaders refused to ask people of their community to take the medicine.”
Dahal himself reached Banke to monitor the mass drug administration programme, which was launched on March 12. Prevalence of lymphatic filariasis or elephantiasis is very high in Banke district. The mosquito-borne parasitic disease is caused by filarial worms transmitted by different kinds of mosquitoes including Culex, Anopheles, and Aedes.
It is the second major infectious disease after leprosy that causes permanent and long-term disability in Nepal.
Health workers complained that people of some communities residing in big cities are not only reluctant to take the medicines distributed in course of the mass drug administration but are sceptical of all health programmes including the Covid-19 vaccination.
“Vaccine coverage of Covid-19 is very low in certain communities,” said Gautam, from the Health Office, Banke.
Dahal of the Epidemiology and Disease Control Division said that the case is not only of Banke but also of Morang, Dang, Kapilvastu and Kailali, among other districts.
Institutional as well as antenatal and postnatal delivery rate is too low. Coverage of the immunisation programme is also low compared to other places, according to health workers.
“We have even tried to take help from religious and local leaders, elected representatives and others,” said Gautam. “But they said they cannot take responsibility for other people.”
The Ministry of Health and Population has committed to administering the Covid-19 vaccine to all eligible people by April 13. But as of Saturday, only 18,703,726 people or 64.1 percent of the total population have been fully vaccinated. Still 33 percent of people above 12 years of age are yet to be fully vaccinated.
“We have decided to inoculate all eligible populations within April 13,” said Dr Samir Kumar Adhikari, joint spokesperson for the Health Ministry. “We have to concede that most of the people who were not inoculated earlier due to whatever reasons have taken the vaccine as of now so finding those who have not taken the jab is not very easy.”
The Ministry of Health and Population had claimed that it would launch a search and immunise programme to meet the target of April 13 but such a programme has not yet been launched. Authorities concerned are unaware of the whereabouts of the people who have not yet taken the Covid-19 vaccine.
“Same strategies will not work, and I have repeated many times that micro planning is needed,” said Dr Baburam Marasini, former director at the Epidemiology and Disease Control Division. “And micro planning is not only necessary in the Covid-19 vaccination drive, but in all programmes of health and other sectors to get the desired results.”
Health Ministry officials concede that hard-to-reach populations exist not only in remote villages but also in big cities and towns. They claim that micro planning is done and awareness drives launched to clear rumours and take people into confidence in most health campaigns, including the vaccination and mass drug administration programmes.




 21.12°C Kathmandu
21.12°C Kathmandu















