Special Supplement
Nepal’s health sector thrived this year but the government should do more to adapt to federalism
During the two-day review of health sector programmes held on 17th and 18th December by the Ministry of Health and Population and various development partners, Nepal’s progress against the National Health Sector Strategy (NHSS) targets and the annual work plan for the fiscal year 2074/75 were addressed.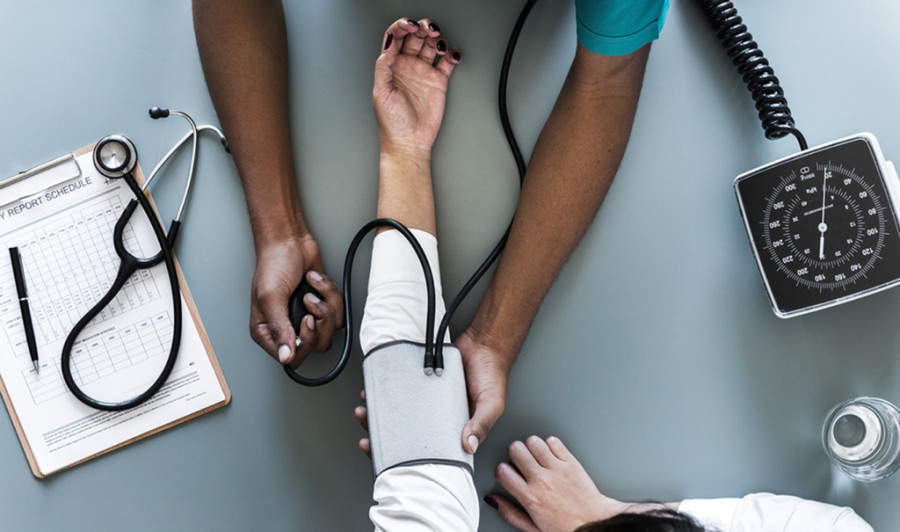
Sudha Sharma
During the two-day review of health sector programmes held on 17th and 18th December by the Ministry of Health and Population and various development partners, Nepal’s progress against the National Health Sector Strategy (NHSS) targets and the annual work plan for the fiscal year 2074/75 were addressed. This year, the National Health Sector Strategy focused on universal health coverage with four strategic directions, namely, equitable access, quality, and multisectoral approach and health sector reform. Efforts have been directed in all these strategic directions with much progress, but the review—as any review should—cautions practitioners to be careful lest the gains made so far could regress.
Progress made
For a start, Nepal achieved the millennium development goal 4 of reducing child mortality and continues to make progress in the area of child health. The approval of the unopposed Safe Motherhood and Reproductive Health Act served as an important intervention in this regard. There has also been steady improvement in access to maternal healthcare. Access to maternal care has also made some progress this year; 58 percent of births today are attended by skilled birth attendants and maternal mortality has declined significantly.
According to the Nepal-WHO Country Cooperation Strategy (CCS) report 2018, there has been a rise in life expectancy and a steady fall in the number of HIV patients, among other developments in the country. Nepal was certified for controlling rubella and congenital rubella syndrome two years ahead of the World Health Organisation (WHO) Southeast Asia’s regional target year of 2020—and one year ahead of the national target of 2019. Nepal has achieved 97 percent reduction of rubella cases against the target of 95 percent in 2008. This is a remarkable achievement, and another milestone in the country’s list of successes against vaccine-preventable diseases.
Over the last two decades, even with scarce resources, the country has made great strides in health care access and quality. The 2012 Resolve Award for Innovative Financing in Improving Maternal Health, the 2010 MDG 5 award for Reduction (by half) in Maternal Mortality between 1990 and 2010, and the 2009 GAVI Alliance Award for Outstanding Performance in Improving Child Health and Immunisation are a few examples.
What’s more, basic health service packages (BHCP) are free to all citizens; the insurance scheme covers costs of services that are beyond the scope of BHCP. The social health insurance act 2074 laid the foundation to make health services accessible to the people and reduce out of pocket expenditure. The social health insurance programme now covers 36 districts (about 10 percent of the target population units) and is expected to cover all the districts by fiscal year 2075/76. However, less than 50 percent of families have reinsured in the subsequent years, indicating that while positive steps have been taken, more work is needed to enhance the popularity and client satisfaction with regards to the social health insurance scheme.
The huge progress Nepal has made in the health sector, especially since 1990, is the result of structural reforms, which included a management information system, both for services and logistics, and a system of ongoing supervision and quality enhancement measures.
Way forward
In order to ensure further gains, intersectoral collaboration, partnerships between the public and the private sector, and more investments in the health sector should be enhanced and encouraged. Furthermore, there seems to be a mismatch between planning and ground realities. Staffing patterns indicate that very few—and often unqualified—people are deployed to local and provincial levels. Local health centres also often lack access to vital infrastructure, undoubtedly affecting their service delivery. Paradoxically, a vast number of trained health professionals have not been given many responsibilities and, for a large part, remain idle in Kathmandu. The provincial ministries should also be equipped with enough human resources and expertise to plan future budgets with a more intentional and evidence-driven approach.
The health sector at large has also not adapted to the federal context. Local health centers have not been given the autonomy they were promised earlier. Further investments need to be made to build the capacities of local health providers. A supportive supervision programme could also help in this regard.
The health team at the local health posts and primary health care centers need technical backstopping which cannot be provided by the administrative staff, or the health staff with lower capacity as is currently present at the local levels. Furthermore, technical backstopping for the local and provincial levels will be essential for logistic management, forecasting, quality assurance and distribution of drugs to all health facilities.
As Nepal continues its ongoing transition to the federal system, the country is likely to face challenges in the process of transferring authority and resources. But the growing pains experienced during this time should be used as an opportunity to focus on quality and innovation.
Sharma is a former secretary at the Ministry of Health and Population.




 21.12°C Kathmandu
21.12°C Kathmandu










