Opinion
Time to wake up
Socio-cultural barriers still make doctors hesitant to specialise in anaesthesiology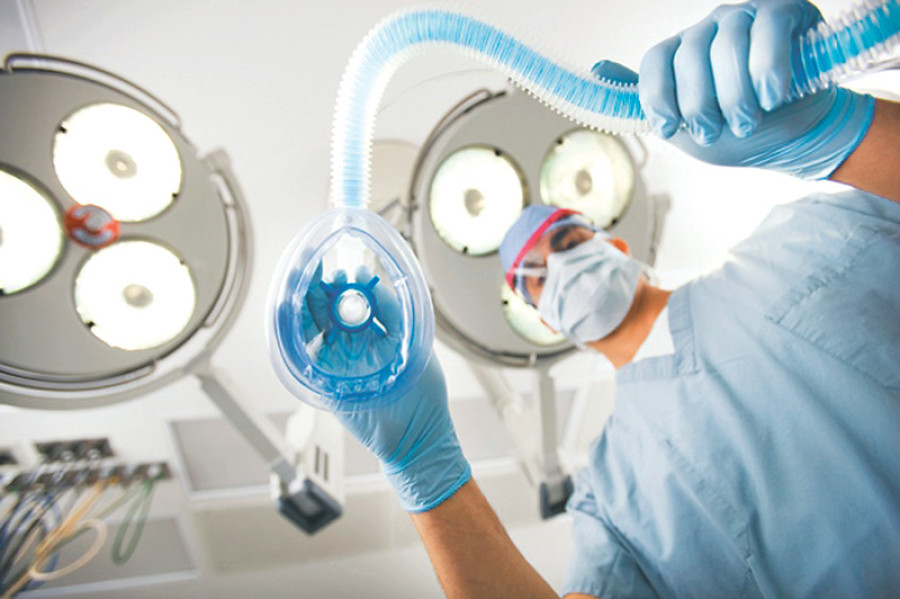
Dr Pawan Hamal
Anaesthesiology is a field that hassuffocated inside the operationtheatre. Graduates specialise in this subject of study with the view to save lives. Global trends document intense competition among anaesthesiologists; winning a postgraduate position inanaesthesia and critical care is highly competitive. In our social context,however, the case is very different.
Recently, the Ministry of Health announced 22 vacancies for anaesthesiologists. Only two applied. We can count the number of specialists working in public hospitals on our fingers, and most are approaching retirement. We rarely find anaesthesiologists working outside Kathmandu Valley. The number of anaesthesiologists in the country now stands around 250. Though the number is slowly growing, people are still hesitant to pursue this area of specialisation.
Public perception
A look into the historical development of anaesthesia in Nepal may provide insight into the trend of low interest in anaesthesiology. While interest in other surgical specialities grew exponentially, the willingness of medical graduates to pursue anaesthesiology as a career was hard hit by socio-cultural issues. An anaesthesiologist was not perceived as a doctor; he was widely regarded as a “gas man” who puts people to sleep. Medical graduates chose specialities that gave them recognition as public figures. Anaesthesiologists were the service providers behind the curtain.
The scarcity of anaesthesiologists was highlighted by a conspicuous lack of trained specialists for surgical procedures and critical care. Only those graduates with weaker results specialised in anaesthesiology as a secondary choice. Though the Health Ministry introduced a provision of extra allowance for anaesthesiologists in a bid to address the shortage, it had little success.
Today, there is only a slight improvement in the public perception of an anaesthesiologist as a “gas man”. Anaesthesiologists are overshadowed by their surgical colleagues; the public has yet to understand that a lack of trained anaesthesiologists can result in clinical problems and even loss of life during surgical procedures.
Existing challenges
A shortage of trained manpower, the prevalent sociocultural context, a lack of proper policy and interest from the government sector, weak societal awareness and improper payment systems are some of the hindrances that need to be addressed. Anaesthesiologists are also to be faulted for their inability to make the public understand their plight. Globally,anaesthesiologists are the leaders of critical care, perioperative care medicine and pain medicine. They have also shown their acumen in the field of policy-making.
The challenges faced by this area of specialisation lie in the shortage of manpower and safe anaesthesia care for the public. To overcome these challenges, there is a need for a stepwise tactical approach. The government has to advocate safe anaesthesia care. This entails, among other measures, raising public awareness through patients’ interaction with anaesthesiologists prior to surgery.
Anaesthesiologists also need to function independently in their practice; they need to show greater willingness to talk with patients, and to charge proper amounts for their service instead of taking cuts from operation charges. Such an environment can only be created through proper policy-making and implementation that help break the socio-cultural barriers and make the care providers more responsive and visible to the public.
Current procedural terminology
The National Anaesthesia Society (NAS) is advocating the use of current procedural terminology in Nepal. It is a scientific system of anaesthesia services and charges that is in place in developed countries. The NAS needs to adapt this system for the Nepali context, making it locally relevant and easily understandable. Backed by government policy, anaesthesia practitioners will be answerable to the state and will be required to interact with patients and provide quality anaesthesia services.
Anaesthesia providers will be an integral part of public hospitals. They will actively participate in overall operative care of patients; the results will be evident in the improved quality of patient care. This will also help break the socio-cultural norms that are biased against anaesthesiologists, encouraging more medical graduates to pursue the field. Once the shortage of anaesthesiologists is addressed, some policy changes could encourage anaesthesiologists to work in rural areas.
More flexible residency selection criteria can eliminate bottlenecks. Once they graduate, financial and non-financial incentives can be provided as a part of an initial programme to those willing to work in rural areas. Integration of the current procedural terminology system in an extended health services policy can be the best way to start this noble cause. Proper infrastructural provision with appropriate oxygen supply systems, operating theatre set-ups, ventilators, assistant staff and administrative support in rural areas can vastly improve the situation of anaesthesiology in Nepal.
Efforts have been made in the past and a number of meetings have been held between the government and the anaesthesia society, but the outcomes have been negligible. Both parties show a lack of willingness to make necessary changes. A pro-active mindset with a visionary approach is needed. Patients from across Nepal are entitled to quality anaesthesia services. It’s time to wake up.
Hamal, an assistant professor ofanaesthesiology at the National Academy of Medical Sciences, is an undersecretary at the Ministry of Health




 19.12°C Kathmandu
19.12°C Kathmandu










