National
The death of yet another burn victim shows how little has changed in the past 20 years
Burns are the second most common injury in rural Nepal, accounting for 5 percent of disabilities, according to the World Health Organisation. Beating and burning are the two most common forms of domestic violence in Nepal, according to women’s rights organisations and several academic studies.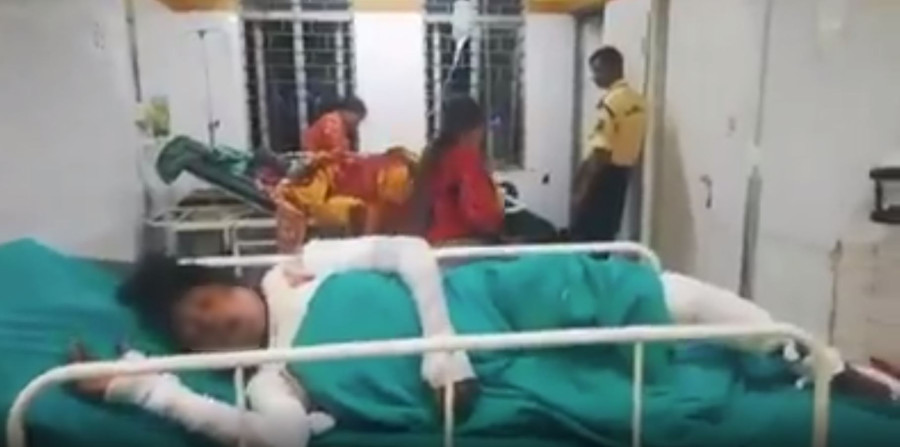
On Friday afternoon, 21-year-old Kanchan Mandal was brought to the burns unit at Sushma Koirala Memorial Hospital in Sankhu, all the way from Dharan. Her heavily bandaged body, covered in an orange saree, was carried out of the ambulance, as her family members looked on, dazed and tired after the long journey from the eastern city. Mandal had burns over 85 percent of her body—half of her face and everything below her shoulders were burnt.
Less than two hours into treatment, Mandal succumbed to her injuries. Doctors who treated her said that losing the crucial 24 hours after the burns resulted in her early death.
“If she had been brought in earlier, maybe she would have lived for another few days,” said Dr Rojina Shilpakar of the Sushma Koirala Hospital.
Since there is no specialised treatment for burns victims anywhere outside of Kathmandu, Mandal had to be transported all the way from Dharan in an ambulance. In Dharan, all doctors could do was clean the wounds on her scalded body and cover them with bandages.
Mandal is among the thousands of Nepalis who lose their lives or end up with severe disabilities after sustaining acute burn injuries, in the absence of timely primary care. The Siraha native was set on fire by her mother-in-law and husband, said a preliminary police investigation.
Burns are the second most common injury in rural Nepal, accounting for 5 percent of disabilities, according to the World Health Organisation. Beating and burning are the two most common forms of domestic violence in Nepal, according to women’s rights organisations and several academic studies. And on Thursday, Kanchan Mandal was yet another name on the growing list of women who succumb to burns because of violence at home.
Nepal has made strides in reducing infant and maternal mortality rates in the last two decades, but the survival rate for acute burn injuries hasn’t changed in the same time frame. In 1998, burns victims in Nepal had little to no chance of survival, and almost two decades later, the situation is just as grim, say experts. According to the Ministry of Health, there were around 56,000 burn injuries in 2018. But doctors say the numbers could be higher since the government doesn’t track burn incidents systematically.
“The numbers have not changed for burns because it has never been a health priority, not just for Nepal but globally as well,” said Shankar Rai, a reconstructive plastic surgeon at the Kirtipur Hospital, which houses the country’s largest burns ward at its Nepal Cleft and Burn Centre.
The 63-year-old surgeon has been at the forefront of bringing attention and resources to this often-neglected public health issue. Rai and his team perform burns-related surgeries almost everyday.
“Our policy is to never turn away any patient, but even then it is sometimes difficult to accommodate many patients with acute burns at the same time,” said Rai.
In the absence of trained health professionals specialising in burns treatment, most think burns treatment is limited to dressing and cleaning wounds, like they did in Dharan for Kanchan Mandal. This can worsen the condition of acute burn patients who go on to develop severe disabilities and muscle contracture. Studies say a lack of awareness about burn prevention, proper first aid, and skin donation has only exacerbated problems in Nepal.
And this is what Rai and his team hope to change with their outreach centres across the country, where they perform thousands of corrective surgeries annually for free, and also talk about the importance of first aid treatment in burns cases. Such treatment is invaluable in towns and villages outside Kathmandu where even the largest hospitals, both public and private, lack expertise to deal with burns cases. But the care and treatment of burns victims in Kathmandu is also limited, with less than a dozen hospitals providing dedicated service.
Until 2015, the burns unit at Bir Hospital was among the handful of places that provided dedicated treatment to people from all over the country. Established two decades ago, it was the country’s first burns ward, and provided victims with intensive care, plastic surgery and physiotherapy as and when needed during the treatment period. Of the 32 beds, eight were set aside for patients with acute burns, who needed intensive care. The burns ward in Bir Hospital had its own operation theatre, a separate dressing and bathing room for patients, and physiotherapy services.
But all that changed after the 2015 earthquakes damaged the Bir Hospital and the burns unit was moved to the sixth floor of the National Trauma Centre, overlooking Tundikhel.
“We aren’t in a position to provide ICU care now,” said Dr Peeyush Dahal of the burns unit. “But we try to do whatever we can.”
Bir Hospital’s lax attitude towards upgrading the burns ward in the four years since the earthquakes has compelled doctors to refer patients with acute burns to other hospitals in the city. They aren’t able to treat critical cases in the absence of physical facilities in the new building, and the number of patients at the burns ward has steadily dropped from about 200 before the earthquake to 60 each year. The number of lives they are able to save has also plummeted.
“If we had an ICU, we could have saved 10 people, but now we are probably only able to save five,” said Dr Dahal.
The absence of proper primary care has affected victims, resulting in kidney failure because of the loss of bodily fluids and contractions leaving them severely disabled. Doctors say the treatment in itself isn’t particularly expensive, but the long period of recovery for burns victims, which includes changing the dressing each day, regular physiotherapy as well as an extended period of hospital stay, tends to add up.
“Most burns victims come from the most marginalised sections of the society, for whom the lack of primary care further burdens long-term treatment and can even result in death,” said Dr Jaswan Shakya of the Sushma Koirala Memorial Hospital, where Kanchan Mandal was being treated.
Speaking to the Post on Friday morning, hours before Mandal was brought in, Shakya said he couldn’t say what condition Mandal was in and how much they could help. As the hours went by and he received updates on her situation, the picture started looking more bleak.
“In Nepal, it’s nearly impossible to save victims with over 40 percent burns. In her [Mandal’s] case, it was over 85 percent,” he said. “There was no way she would’ve survived.”




 18.12°C Kathmandu
18.12°C Kathmandu














