Health
Behind the frequent measles outbreaks
Low uptake of vaccines is the main reason. The World Health Organisation on Friday called on countries to take urgent measures against measles.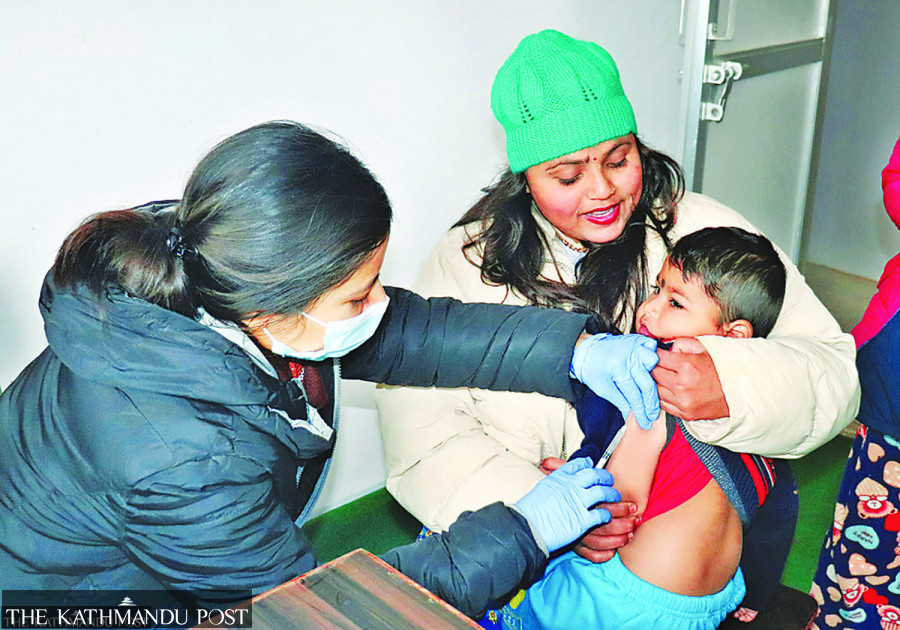
Arjun Poudel
Nepalgunj Sub-metropolitan City has been witnessing a massive measles outbreak over the last two weeks. The contagious viral disease, which killed a 30-month-old toddler and has infected over 130 people, has already spread in 12 of the 23 wards of the sub-metropolis.
Health authorities in Banke have been launching mass vaccination drives in the disease-hit wards of the city in which children aged between six months and 15 years are being jabbed with the measles vaccine. Infection has been seen in the adult population as well, but they are only getting post-symptomatic treatment.
The outbreak has occurred in an area that was declared ‘fully immunised’ in March 2021.
Child health experts in Nepal questioned the authenticity of government agencies’ claims of fully-immunised local units and districts and seriousness of the three tiers of government towards achieving the country’s health goals.
Here’s all about Nepal’s current childhood vaccination status and the reason for the frequent measles outbreaks.
What is measles?
Measles is a contagious disease caused by a virus of the paramyxovirus family. It is transmitted through fluids from the nose, mouth or throat of infected persons and through air. The virus infects the respiratory tract, then spreads throughout the body. It remains a big cause of death among young children globally despite the availability of a safe and effective vaccine, according to the World Health Organisation.
Measles history in Nepal
Measles was endemic in Nepal. In the past, hundreds of children died every year in the country from the potentially fatal contagion.
Routine measles vaccination in Nepal began in 1979, starting with three districts. The campaign was extended nationwide after 10 years. Despite measles vaccines being included in the regular immunisation list, an average of 90,000 cases were recorded every year from 1994 to 2004.
“I was deputed to Doti after deaths of over 300 children from measles infection there some 35 years ago,” said Dr Baburam Marasini, former director at the Epidemiology and Disease Control Division. “I remember we had admitted and treated more than 80 children in a 15-bed hospital.”
With the increase in vaccine coverage, both infection and death rates from the virus declined significantly. Still, measles continues to stalk many children across the country.
The vaccine
Measles can be prevented through immunisation. The best way to protect against the deadly disease is to get the measles-rubella (MR) shots. The government has included the MR shots in its regular immunisation programme and offers the vaccine free of cost. Children get two doses of vaccine—in nine months and in 15 months—under the programme. Apart from this, health authorities also launch a nationwide mass vaccination drive every four years targeting children who missed the vaccine doses in regular immunisation programmes. All children under five are administered the MMR vaccine during the campaign.
Why frequent outbreaks?
Currently, Nepalgunj Sub-metropolis has been grappling with a massive measles outbreak. Such incidents were previously reported from Kapilvastu, Dang, Dhading, Kathmandu and Morang, among other districts.
Low vaccination coverage, internal migration, lack of public awareness on the importance of vaccines and government apathy are attributed to regular outbreaks of measles in the districts, according to health experts.
Public health experts say most measles outbreaks have been reported among the marginalised and religious communities—Muslims and Catholics—as well as other backward groups where the level of awareness of regular immunisation is low. Rumours about measles vaccines causing impotence and high fever are also still rife in these communities.
The vaccine coverage rate is low in some Muslim communities, as they believe that gelatine derived from pigs is included in the vaccines. Some from the Catholic Christian community believe they don’t need vaccines as God takes care of them. Also, some elites in major cities apparently reckon they can do without vaccination. Moreover, working class people who go from place to place are also being deprived of vaccination.
“When all children are not immunised, risks of disease outbreaks increase,” said Dr Jhalak Gautam, former chief of the Immunisation Section at the Family Welfare Division under the Department of Health Services. “We must make every effort to increase the vaccine coverage.”

Nepal’s goal of measles elimination
Nepal had committed to eliminating measles by 2023. But the outbreak of the deadly disease at the start of 2023 shows that the country is nowhere near meeting the measles elimination target. The previous deadline of 2019 had to be extended due to the failure to meet the target.
To declare measles as eliminated, the number of cases should be less than five in every million people throughout the year.
“To achieve measles elimination status, over 95 percent of the total children need to be immunised with both doses of vaccine and no children should miss the vaccine,” said Dr Jhalak Sharma, former chief of the Immunisation section at the Family Welfare Division of the Department of Health Services.
Nepal’s vaccination status
A recent report of the Nepal Demographic and Health Survey-2022 carried out by the Ministry of Health and Population shows that four percent of children in the 12–23 month age group have received no vaccine.
This figure was just one percent in 2016, and the rapid surge in the number of unvaccinated children poses a serious threat to the country’s achievements in immunisations made over the years through huge investments, child health experts warn.
The study shows that overall, 80 percent of children aged 12–23 months are fully vaccinated with basic antigens. The measles-rubella vaccine uptake rate is 89 percent. The percentage of children aged 12–23 months who are fully vaccinated (received all the basic antigens) has fluctuated over the time, rising from 43 percent in 1996 to a peak of 87 percent in 2011, then decreasing to 78 percent in 2016, and again increasing slightly to 80 percent in 2022.
Experts’ take
Child health experts say the increase in the number of children who did not take any vaccine from one percent to four percent in a five-year period is alarming.
“We are at a risk of outbreaks of multiple vaccine-preventable diseases. All our achievements in child health are at risk,” said Gautam, the former chief of the Immunisation Section at the Family Welfare Division of the Department of Health Services. “After the declaration of a fully immunised district, the vaccination programme perhaps got less priority. Without developing a system that ensures that no child misses the vaccines, these types of outbreaks won’t stop.”
The experts suggest micro-planning to ensure no child misses the vaccine, improvement of preparedness to respond to the outbreaks and better coordination among the concerned agencies under all three tiers of governments, as well as with international partners, including UN bodies like WHO and UNICEF.
Status in South-East Asia region
According to UNICEF, five out of the region’s 11 countries (Bhutan, DPR Korea, Maldives, Sri Lanka and Timor-Leste) have eliminated Measles and two countries (the Maldives and Sri Lanka) have eliminated Rubella as well.
But the potentially deadly disease is still being spotted in Nepal, Indonesia, Myanmar, Bangladesh, India and Thailand.
WHO on measles risks in the region
The World Health Organisation South-East Asia Region on Friday called on countries to take urgent and accelerated measures against Measles which is on the rise with nearly nine million children in the region having missed vaccination against the killer disease in the last two years.
Issuing a press statement on the 12th anniversary of the last case of wild poliovirus detected in the region, Regional Director Dr Poonam Khetrapal Singh said a strong political commitment, determination, focussed and concerted efforts and community support that marked efforts for polio elimination are now urgently needed to stop and prevent measles outbreaks and called for accelerated efforts to eliminate the disease.
Measles and rubella elimination is the flagship priority programme of WHO South-East Asia Region. The region recorded 73 percent reduction in measles deaths and 64 percent reduction in measles cases between 2014 and 2021.
“The decline in vaccine coverage, and interruptions and delays in immunisation and surveillance activities due to Covid-19, leaves the region susceptible to large outbreaks, and off track for the 2023 target of measles and rubella elimination,” said the regional director. “We need to urgently close immunity gaps with tailored approaches for highest impact, such as through catch-up campaigns, and strengthening of the routine immunisation with better micro-planning.”




 21.12°C Kathmandu
21.12°C Kathmandu















